Last Updated on April 25, 2026
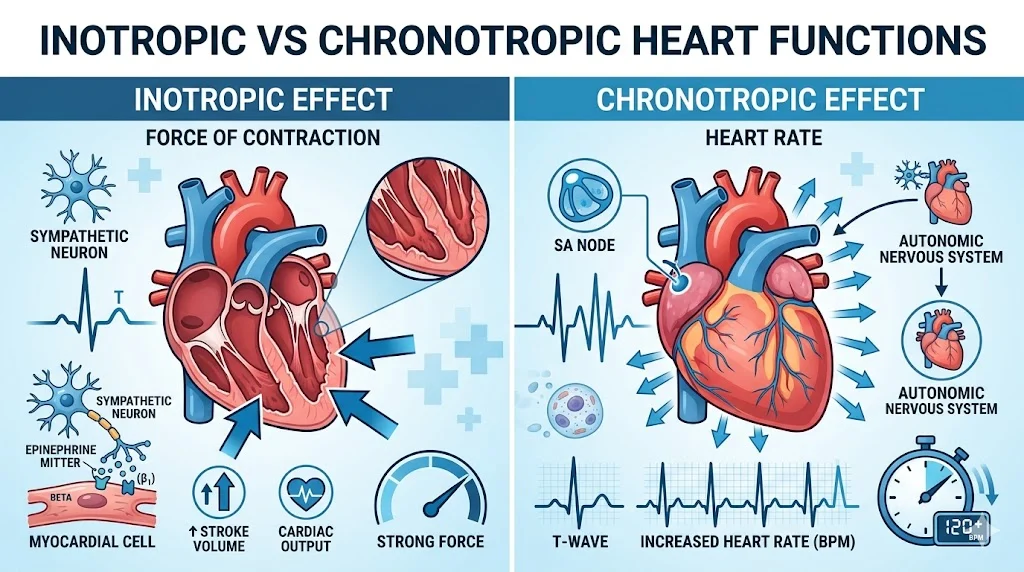
Inotropic vs chronotropic refers to two different ways the heart’s function can be affected. Inotropic action changes the force of heart muscle contraction, while chronotropic action changes the heart rate. These concepts are essential in cardiology, especially when treating heart failure, arrhythmias, and shock.
Understanding inotropic vs chronotropic effects helps doctors choose the right medications to control heart strength and heart rate safely.
The human heart is a powerful pump that works nonstop to keep us alive. But sometimes, its rhythm or strength can change due to disease, stress, or medication. This is where the concepts of inotropic vs chronotropic effects become very important in medicine.
Many students, nurses, and even patients get confused between these two terms. They sound similar but describe very different functions of the heart. One affects how strongly the heart beats. The other affects how fast it beats.
Doctors use these terms every day when treating heart failure, low blood pressure, or abnormal heart rhythms. Medicines like beta-blockers, dopamine, and dobutamine directly influence inotropic and chronotropic actions.
In this guide, you will learn the difference between inotropic vs chronotropic in a simple and clear way. We will explore definitions, examples, clinical uses, and common mistakes. Even if you are a beginner in medical science, this article will help you understand these concepts easily and confidently.
Quick Answer Overview of Inotropic vs Chronotropic
The terms inotropic vs chronotropic describe two different cardiac effects:
- Inotropic effect: Changes the force of heart contraction
- Chronotropic effect: Changes the heart rate
In simple terms:
- Inotropic = How strong the heart beats
- Chronotropic = How fast the heart beats
Both are controlled by the autonomic nervous system and medications used in cardiology.
Definition and Explanation of Inotropic vs Chronotropic
What is Inotropic?
The term inotropic refers to the strength of heart muscle contraction. It comes from “ino” meaning muscle and “tropic” meaning change.
- Positive inotropic effect increases contraction strength
- Negative inotropic effect decreases contraction strength
Example:
- Dobutamine increases heart strength (positive inotrope)
- Beta-blockers may reduce contractility (negative inotrope)
Inotropic action is crucial in conditions like heart failure, where the heart is too weak to pump blood effectively.
What is Chronotropic?
The term chronotropic refers to the heart rate or timing of heartbeats.
- Positive chronotropic effect increases heart rate
- Negative chronotropic effect decreases heart rate
Example:
- Adrenaline increases heart rate (positive chronotrope)
- Beta-blockers slow heart rate (negative chronotrope)
Chronotropic control is important in conditions like bradycardia (slow heart rate) and tachycardia (fast heart rate).
Key Differences Between Inotropic vs Chronotropic
Below is a simple comparison table to make inotropic vs chronotropic easier to understand:
| Feature | Inotropic Effect | Chronotropic Effect |
| Definition | Force of contraction | Heart rate |
| Focus | Strength of heartbeat | Speed of heartbeat |
| Measured by | Stroke volume | Beats per minute |
| Controlled by | Cardiac muscle contractility | SA node activity |
| Example drugs | Dobutamine, digoxin | Atropine, beta-blockers |
| Clinical use | Heart failure treatment | Arrhythmia management |
Mechanism of Inotropic vs Chronotropic Effects
Autonomic Nervous System Role
The autonomic nervous system controls both inotropic vs chronotropic functions.
It has two parts:
- Sympathetic nervous system
- Parasympathetic nervous system
Sympathetic System
- Increases both inotropic and chronotropic effects
- Releases norepinephrine and epinephrine
- Stimulates beta-1 receptors in the heart
Effects:
- Stronger heart contractions (positive inotropy)
- Faster heart rate (positive chronotropy)
Parasympathetic System
- Decreases heart activity
- Uses acetylcholine
- Acts mainly through the vagus nerve
Effects:
- Slower heart rate (negative chronotropy)
- Mild reduction in contraction strength
Beta-1 Receptors and Heart Function
Beta-1 receptors play a central role in inotropic vs chronotropic control.
When stimulated:
- Increase calcium influx in heart cells
- Enhance contraction strength
- Increase heart rate
This is why drugs affecting beta receptors are widely used in cardiology.
Advantages and Disadvantages of Inotropic vs Chronotropic Effects
Positive Inotropic Effects
Advantages:
- Improves blood circulation in heart failure
- Supports cardiac output in shock
- Helps maintain blood pressure
Disadvantages:
- Can increase oxygen demand
- Risk of arrhythmias
- May strain the heart long-term
Positive Chronotropic Effects
Advantages:
- Treats slow heart rate (bradycardia)
- Improves cardiac output in emergencies
- Enhances blood flow during stress
Disadvantages:
- Can cause palpitations
- Increases myocardial oxygen demand
- May worsen ischemic heart disease
Real-World Examples of Inotropic vs Chronotropic Effects
Medications with Inotropic Effects
- Dobutamine: Strong positive inotrope used in heart failure
- Digoxin: Increases contractility in controlled doses
- Dopamine: Dose-dependent inotropic effects
Medications with Chronotropic Effects
- Atropine: Increases heart rate in bradycardia
- Beta-blockers (Metoprolol): Reduce heart rate
- Epinephrine: Increases both heart rate and force
Clinical Scenario Example
A patient with heart failure may receive:
- Dobutamine → improves contraction (inotropic effect)
A patient with bradycardia may receive:
- Atropine → increases heart rate (chronotropic effect)
Clinical Importance of Inotropic vs Chronotropic Effects
Understanding inotropic vs chronotropic is essential in many medical situations:
Heart Failure
- Needs positive inotropic support
- Helps pump blood efficiently
Arrhythmias
- Requires chronotropic control
- Stabilizes heart rhythm
Shock Conditions
- Requires both inotropic and chronotropic support
- Maintains blood pressure and circulation
Intensive Care Units (ICU)
- Continuous monitoring of both effects
- Drug titration based on heart response
Regional and Global Usage in Medical Practice
The concept of inotropic vs chronotropic is globally used in:
- USA and Europe: Advanced cardiac life support protocols
- Asia: Medical education emphasizes exam-based understanding
- Middle East: Clinical cardiology training uses drug-based examples
- Pakistan and South Asia: Strong focus in MBBS pharmacology and physiology
Despite regional differences, the physiological principles remain the same worldwide.
Common Mistakes in Understanding Inotropic vs Chronotropic
Mistake 1: Thinking both are the same
- Correction: Inotropic affects strength, chronotropic affects rate
Mistake 2: Confusing drug effects
- Correction: Some drugs affect both, not just one
Mistake 3: Ignoring dose dependence
- Correction: Dopamine can be inotropic at low doses and chronotropic at high doses
Mistake 4: Mixing up terms in exams
- Correction: Remember “I = Intensity (force), C = Count (rate)”
Exercises with Answers
Exercise 1
What does a positive inotropic effect do?
Answer: Increases the force of heart contraction
Exercise 2
Which system increases chronotropic activity?
Answer: Sympathetic nervous system
Exercise 3
Is atropine inotropic or chronotropic?
Answer: Chronotropic (increases heart rate)
Exercise 4
What is the main effect of beta-blockers on the heart?
Answer: Negative chronotropic and negative inotropic effects
Exercise 5
Name one drug that increases inotropy.
Answer: Dobutamine
Related Concepts and Comparisons
Inotropic vs Dromotropic
- Inotropic: contraction strength
- Dromotropic: conduction speed through AV node
Chronotropic vs Bathmotropic
- Chronotropic: heart rate
- Bathmotropic: excitability of cardiac cells
Cardiac Output Relationship
Cardiac output depends on:
- Heart rate (chronotropic effect)
- Stroke volume (inotropic effect)
FAQs
What is the main difference between inotropic vs chronotropic?
Inotropic affects heart contraction strength, while chronotropic affects heart rate.
Can a drug affect both inotropic and chronotropic functions?
Yes, drugs like epinephrine affect both.
What is a positive inotropic drug?
A drug that increases heart contraction strength, like dobutamine.
What is a negative chronotropic effect?
It reduces heart rate, commonly seen with beta-blockers.
Why are inotropic drugs used in heart failure?
They improve weak heart pumping ability.
Which is more important, inotropic or chronotropic?
Both are important and depend on the medical condition.
Does exercise affect inotropic vs chronotropic functions?
Yes, exercise increases both heart rate and contraction strength.
Are chronotropic drugs safe?
They are safe when used correctly but require monitoring.
What happens if both effects increase too much?
It can lead to arrhythmia or cardiac stress.
How do doctors choose between inotropic and chronotropic therapy?
They evaluate heart rate, blood pressure, and cardiac output.
Conclusion
The concept of inotropic vs chronotropic is essential in understanding how the heart works and how it responds to different conditions and medications. Inotropic effects control the strength of heart contractions, while chronotropic effects control the heart rate. Both are regulated by the autonomic nervous system and influenced by various drugs used in cardiology.
In clinical practice, these concepts help doctors manage heart failure, arrhythmias, and shock effectively. A clear understanding of these effects also improves safe medication use and patient outcomes.
For students and healthcare professionals, mastering inotropic vs chronotropic is not just theoretical but practical knowledge that is applied daily in hospitals and emergency care. Always remember: strength is inotropic, speed is chronotropic.

Victoria Lane is a grammar-focused writer at GramBrix.com, passionate about helping readers master the rules of language. She provides clear explanations and practical examples that make writing more accurate, polished and confident.